Parkinson's disease: practical guide for patients and carers
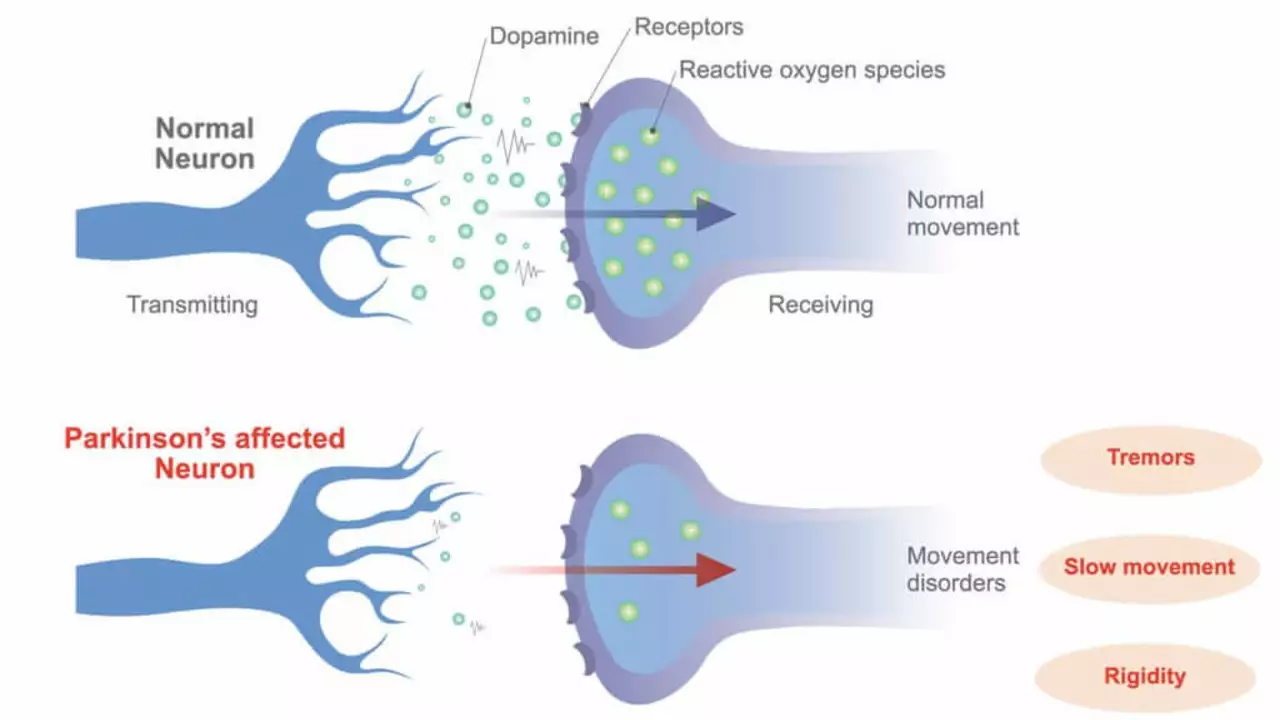
Parkinson's disease is a movement disorder caused by loss of dopamine-producing brain cells. It usually starts slowly and gets worse over years. You don't need a textbook to act on early signs—knowing the common symptoms and simple steps to manage them makes a big difference.
Common symptoms to watch for
Tremor at rest (a shaking hand) is classic, but not everyone has it first. Slowness of movement (bradykinesia), stiffness, and a shuffling walk are frequent. Non-motor issues matter just as much: sleep problems, constipation, smell loss, low mood, and urinary changes. If you notice a clear change in movement or day-to-day abilities, write down when it started and bring that to your doctor.
Medications and how to manage them
Levodopa is the most effective medicine for Parkinson's. It turns into dopamine in the brain and eases movement. Other options include dopamine agonists and MAO-B inhibitors. Each drug has trade-offs: some cause sleepiness, hallucinations, or impulse control issues (like gambling). Keep a medication diary noting dose times and how you feel—this helps your neurologist tweak timing to reduce 'off' episodes.
Timing matters. Take levodopa on schedule for best effect. Avoid sudden stops without medical advice. Some common drugs (like metoclopramide for nausea) can make Parkinson's worse—always check with your movement-disorder specialist or pharmacist before starting any new medicine.
If medications become less predictable you might hear about advanced options: controlled-release formulations, pump delivery, or deep brain stimulation. These are for people whose symptoms don’t respond well to pills. Ask a specialist about risks and benefits; they're not for everyone.
Exercise is medicine. Regular walking, balance work, tai chi, and cycling improve mobility and mood. Speech therapy helps if voice and swallowing change. Occupational therapists suggest small home tweaks that make daily tasks easier.
Practical home and carer tips: remove loose rugs, add grab rails, use non-slip mats, and make lighting brighter in hallways. Encourage short, frequent movement sessions rather than one long push. If freezing happens (feet feel glued), try weight shifts, stepping over a line on the floor, or turning around slowly. For swallowing problems, sit upright and take small bites.
Prepare for appointments: keep a list of symptoms, medication times, side effects, and recent falls. Bring a trusted person if memory or communication is affected. Ask about local support groups—talking with others who live with Parkinson's often gives useful, real-life tips.
Red flags to seek urgent care: sudden confusion, severe trouble breathing, choking repeatedly, or a big drop in blood pressure. For slow changes, a movement-disorder neurologist gives the most focused care and treatment planning.
Parkinson's is different for everyone. Small, steady changes—timed medications, tailored exercise, safe home changes, and good specialist support—help you keep control of day-to-day life.
The Role of Rasagiline in Slowing Parkinson's Disease Progression
In my latest blog post, I delve into the significant role that Rasagiline plays in slowing the progression of Parkinson's disease. This drug, often used as a primary treatment, works by increasing the levels of dopamine in the brain to help improve motor function. Not only does it alleviate symptoms such as tremors and stiffness, but recent studies also suggest that it may slow disease progression. However, it's important to note that while Rasagiline shows promise, it's not a cure and should be used as part of a comprehensive treatment plan. Stay tuned for more health-related insights and breakthroughs.
