Inflammatory bowel disease — signs, daily care, and smart next steps
About 1.6 million Americans live with inflammatory bowel disease (IBD), a term that covers Crohn’s disease and ulcerative colitis. If you or someone close to you is dealing with frequent stomach pain, bloody stools, or sudden weight loss, that could be IBD. You don’t need fancy tests to start paying attention—simple tracking and a quick plan can make a big difference.
What to watch for
IBD symptoms vary, but these are the red flags: ongoing belly pain, urgent or frequent bowel movements, visible blood in stool, unexplained fatigue, and sudden weight loss. If you have fever with abdominal pain, signs of dehydration, or can't keep food down, get urgent medical care.
Keep a short symptom log for two weeks: note meals, stress, meds, bowel frequency, and pain level. That log makes clinic visits far more useful and helps your doctor spot triggers faster.
Practical tips for daily life
Simple changes often help control flares and reduce surprises. Start with food and meds, then add small lifestyle tweaks.
- Diet basics: There’s no one-size-fits-all IBD diet. Try a low-residue or low-fiber plan during flares to ease symptoms, then reintroduce foods slowly. For ideas on food and cancer risk or general diet guidance, see our piece on Nutrition and Tumor Growth.
- Pain and fever: Use acetaminophen for pain and fever when advised by your clinician—avoid NSAIDs unless your doctor says otherwise (NSAIDs can sometimes flare IBD). For more about choosing pain meds, read Acetaminophen Facts and alternatives to Meloxicam.
- Supplements: Some people find benefit from certain supplements, but always check first—some can interact with prescription drugs. See our articles on rose geranium oil, black mulberry, and lentinan for background, then ask your clinician.
- Medication access: If you need to buy meds online or across borders, know the rules and risks. Our guide on Cross-Border Drug Purchasing explains customs and safety tips.
During appointments, bring your symptom log, a list of current meds (including supplements), and questions about long-term risks like bone health or surgery. Ask about vaccination status, especially for infections that can be worse if you’re on immune-suppressing drugs.
Managing IBD is rarely about a single fix. It’s a mix of watching patterns, steady communication with your care team, and practical daily moves—like adjusting meals or timing medications—that add up. If something feels off, speak up early; catching a flare sooner usually means simpler treatment and fewer days lost to pain or worry.
The Connection between Chronic Diarrhea and Inflammatory Bowel Disease (IBD)
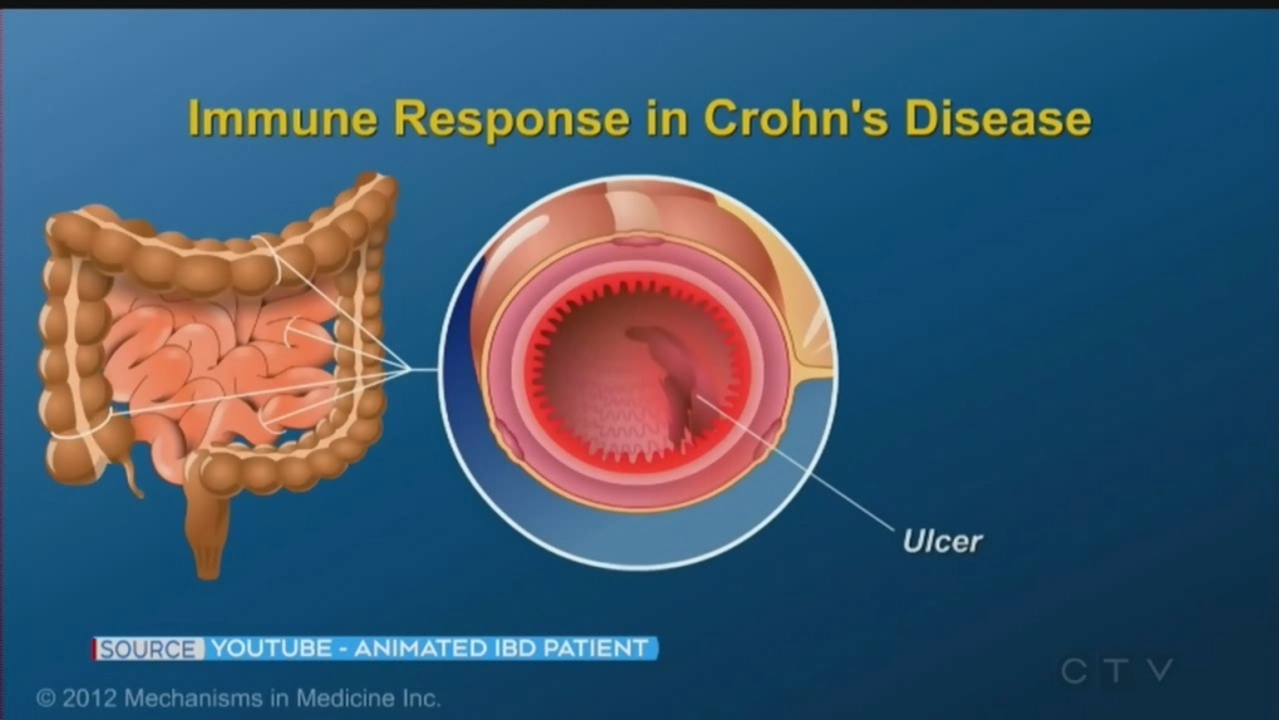
As a blogger, I've recently delved into the connection between chronic diarrhea and Inflammatory Bowel Disease (IBD). I've discovered that chronic diarrhea can be a significant symptom of IBD, as it is caused by inflammation in the digestive tract. This inflammation can lead to various complications, such as pain, malnutrition, and even a higher risk of colon cancer. It's essential for those experiencing persistent diarrhea to consult a medical professional for proper diagnosis and treatment. By managing IBD effectively, patients can relieve their chronic diarrhea and improve overall quality of life.
