IBD (Inflammatory Bowel Disease): What to Watch For and What to Do
About 3 million adults in the U.S. live with IBD — Crohn’s disease or ulcerative colitis — and a lot of people still get stuck guessing what to do next. If you’re dealing with unpredictable belly pain, urgent trips to the bathroom, or unexplained weight loss, this page gives clear, practical steps you can use right away.
Spotting IBD: common signs and first steps
IBD often shows up as belly pain, persistent diarrhea, blood in stools, loss of appetite, or fatigue that won’t quit. If you have those symptoms for more than a few weeks, see a clinician. They’ll likely recommend blood tests, stool checks for inflammation or infection, and a colonoscopy to get a clear look. Early diagnosis matters — it can prevent complications and get you on a treatment plan faster.
When you go to the doctor, bring a short symptom diary: what you ate, pain level, bathroom trips, and any medication or supplements. That simple record helps your care team spot patterns and avoid repeated tests.
Treatment basics and daily management
Treatment aims to stop inflammation, relieve symptoms, and keep you in remission. Options include aminosalicylates, corticosteroids for short-term flares, immunomodulators, and biologic therapies. Some people need surgery when medication can’t control complications. Talk with your gastroenterologist about risks and realistic goals for treatment — ask how success will be measured and what side effects to watch for.
Daily life matters. There’s no one-size-fits-all diet for IBD, but simple actions help: keep a food diary, avoid foods that trigger symptoms for you, stay hydrated, and consider a registered dietitian if you’re losing weight. During flares, lower-fiber and bland foods can ease symptoms; once stable, aim for balanced nutrition and protein to support healing.
Medication safety is key. Check interactions before adding supplements or new prescriptions — RXConnected has guides on drug interactions and buying meds safely online. If cost is a problem, explore patient assistance programs, generics, or verified discount services rather than risky overseas sellers.
Mental health is part of the picture. Anxiety and depression are common with IBD. Support groups, therapy, and peer communities can help you cope and find practical tips from people who get it. If pain or symptoms suddenly worsen, or you get a high fever, severe bleeding, or signs of dehydration, seek emergency care.
If you want more, RXConnected has articles on nutrition, safe online pharmacy buying, and support resources. Bookmark this page and use it as a quick checklist when you speak with your care team — clear notes beat confusion every time.
The Connection between Chronic Diarrhea and Inflammatory Bowel Disease (IBD)
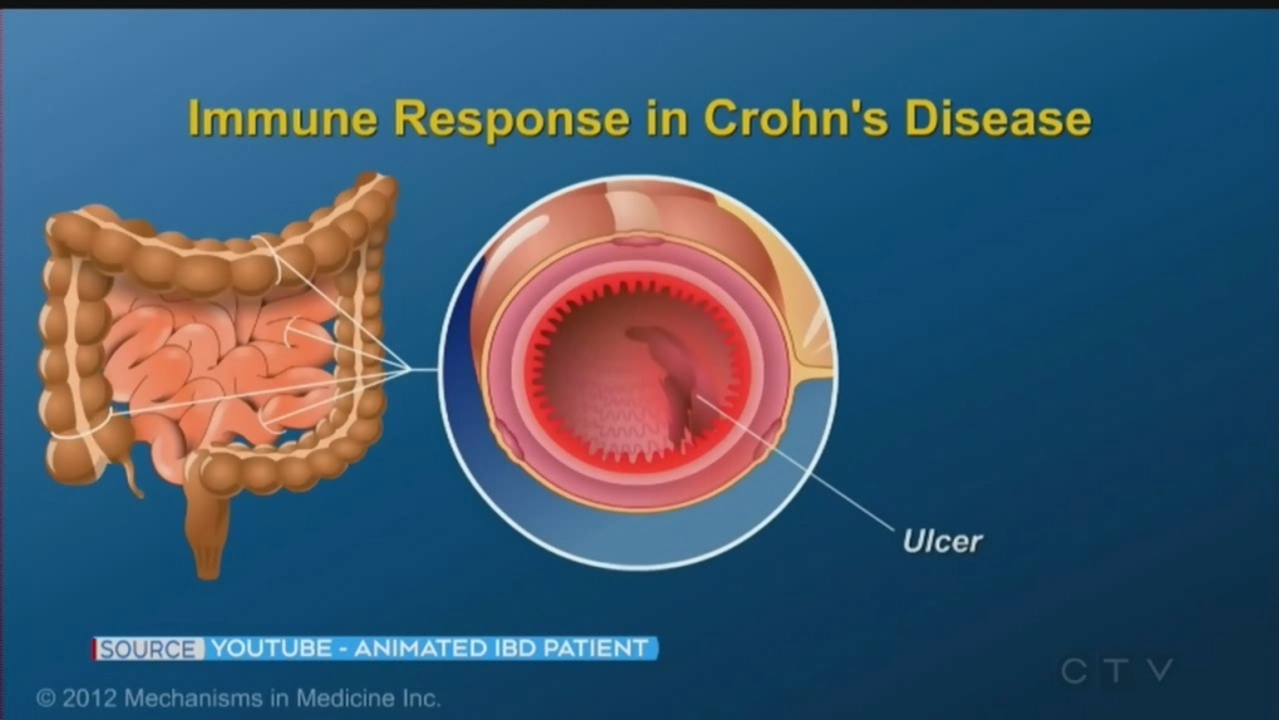
As a blogger, I've recently delved into the connection between chronic diarrhea and Inflammatory Bowel Disease (IBD). I've discovered that chronic diarrhea can be a significant symptom of IBD, as it is caused by inflammation in the digestive tract. This inflammation can lead to various complications, such as pain, malnutrition, and even a higher risk of colon cancer. It's essential for those experiencing persistent diarrhea to consult a medical professional for proper diagnosis and treatment. By managing IBD effectively, patients can relieve their chronic diarrhea and improve overall quality of life.
