Disease Progression: What It Means and What You Can Do
Disease progression simply means a condition is changing over time — getting better, getting worse, or moving through defined stages. That change looks different depending on the illness. For example, cancer progression often means tumor growth or spread; in diabetes it shows up as rising A1c and new complications; in COPD progression means worsening breathlessness and lower lung function. Knowing how progression works helps you spot problems early and act fast.
How progression is tracked
Doctors use a mix of your story, exams and tests. You might notice new symptoms or a steady decline in function — those are clues. Clinicians confirm with labs (blood sugar, kidney markers, inflammatory markers), imaging (X-ray, CT, MRI), or function tests (spirometry for lungs, eGFR for kidneys, neurologic exams for brain disorders). Staging systems — like cancer stages or heart failure classes — give a snapshot of where you are and how aggressive treatment should be. Keep a simple symptom diary: dates, what changed, what made it better or worse. That record often tells the doctor more than you think.
Practical ways to slow or manage progression
Not every disease can be stopped, but many can be slowed or controlled. Start with basics: stick to prescribed meds, go to follow-up visits, and get recommended tests on time. Small daily habits add up — quit smoking, move when you can, eat a balanced diet, and keep weight in a healthy range. For conditions linked to diet or lifestyle (like some cancers or heart disease), targeted changes matter — reducing processed meat and added sugar, increasing vegetables, and keeping alcohol in check can reduce risks noted in recent nutrition reviews.
Ask your clinician about proven interventions: vaccines, blood pressure control, glucose management, or specific drugs that slow decline. If mobility or thinking is changing, consider rehab or cognitive therapy early — those services can preserve function longer than waiting until things are worse. Mental health matters too: anxiety and depression make self-care harder and can speed decline, so get help when you need it.
Know when to escalate care. Sudden new weakness, severe pain, confusion, difficulty breathing, or signs of infection need prompt attention. If your daily life gets harder — stairs become impossible, or you can’t manage meds safely — talk to your team about home support, changes in treatment, or palliative options. Planning ahead (advance directives, clear medication lists) saves stress later.
Tracking progression is a team effort. You, your family, and your healthcare providers all add pieces to the picture. Keep notes, ask clear questions at appointments, and push for tests or referrals if something feels off. Small steps taken early often have the biggest impact on how the story unfolds.
The Role of Rasagiline in Slowing Parkinson's Disease Progression
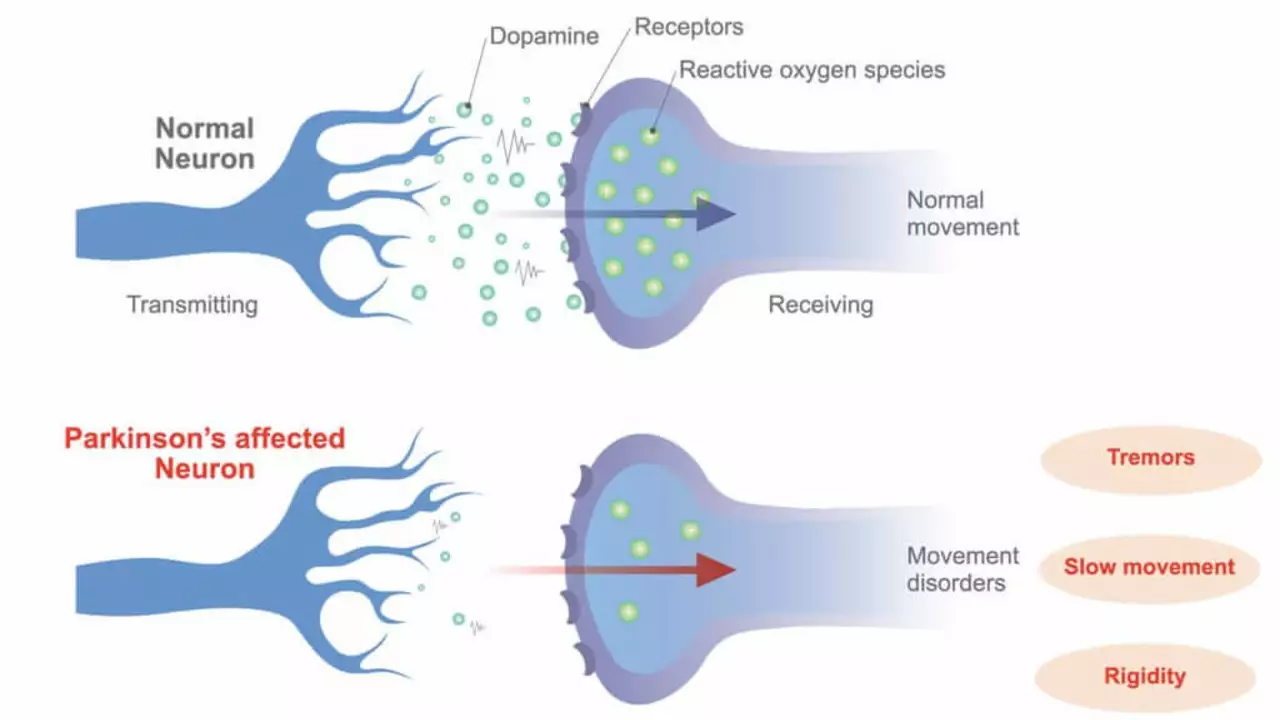
In my latest blog post, I delve into the significant role that Rasagiline plays in slowing the progression of Parkinson's disease. This drug, often used as a primary treatment, works by increasing the levels of dopamine in the brain to help improve motor function. Not only does it alleviate symptoms such as tremors and stiffness, but recent studies also suggest that it may slow disease progression. However, it's important to note that while Rasagiline shows promise, it's not a cure and should be used as part of a comprehensive treatment plan. Stay tuned for more health-related insights and breakthroughs.
