Chronic diarrhea: what it is and what to do next
Chronic diarrhea means loose or watery stools that last more than four weeks. That’s long enough to hurt your daily life, sap your energy, and cause weight loss or dehydration. You don’t have to accept it—there are clear steps to find a cause and treat it.
Common causes you should know
Start by thinking about timing and triggers. Common causes include irritable bowel syndrome with diarrhea (IBS-D), inflammatory bowel disease (Crohn’s or ulcerative colitis), persistent infections (Giardia or other parasites), medication side effects (metformin, SSRIs, antibiotics, magnesium), food intolerances (lactose, fructose), and malabsorption like celiac disease. Less common causes are microscopic colitis, bile acid diarrhea after gallbladder removal, and small intestinal bacterial overgrowth (SIBO).
Look for clues: blood or mucus in stool points more toward inflammation or infection. Weight loss and high fever are red flags for a serious condition. If symptoms started after travel or antibiotics, an infection or C. difficile could be the culprit.
Practical tests and what they tell you
Your doctor will usually start with simple tests. Stool tests can find infections, parasites, or excess fat (steatorrhea). Blood tests check for inflammation (CRP), anemia, and celiac disease antibodies (tTG). Fecal calprotectin helps separate IBS from inflammatory bowel disease. If those don’t give answers, expect a colonoscopy to look directly at the bowel and take biopsies for microscopic colitis or IBD. Breath tests can detect SIBO or lactose intolerance.
Bring a list of all medicines, recent travel, and a short food diary to your appointment. That saves time and points the tests in the right direction.
Treatment targets the cause. For infections you may get antibiotics or antiparasitics. If bile acid diarrhea is diagnosed, bile acid sequestrants like cholestyramine help. Loperamide reduces stool frequency and is useful short term for symptom control. For IBS-D, low‑FODMAP diet changes, peppermint oil, and certain prescription drugs or probiotics can work. Microscopic colitis often responds to budesonide. Celiac disease requires a lifelong gluten-free diet.
Hydration matters: drink oral rehydration solution or salty fluids if you’re losing a lot of water. Avoid caffeine, alcohol, and sugary drinks that can make stools worse. Try a temporary pause on dairy and high‑FODMAP foods while you’re troubleshooting.
When should you get urgent care? Go now if you have severe belly pain, fever over 101.5°F (38.6°C), repeated vomiting, signs of dehydration (dizziness, dark urine), or large amounts of blood in stool. Otherwise, if symptoms persist more than two weeks or you’re losing weight, see your primary care doctor or a gastroenterologist.
Tracking stool patterns, recent changes, and treatments makes follow-up more effective. With the right tests and targeted treatment, most causes of chronic diarrhea can be managed or cured. Start with good notes, get basic tests, and push for a clear diagnosis so you can get back to normal life.
The Connection between Chronic Diarrhea and Inflammatory Bowel Disease (IBD)
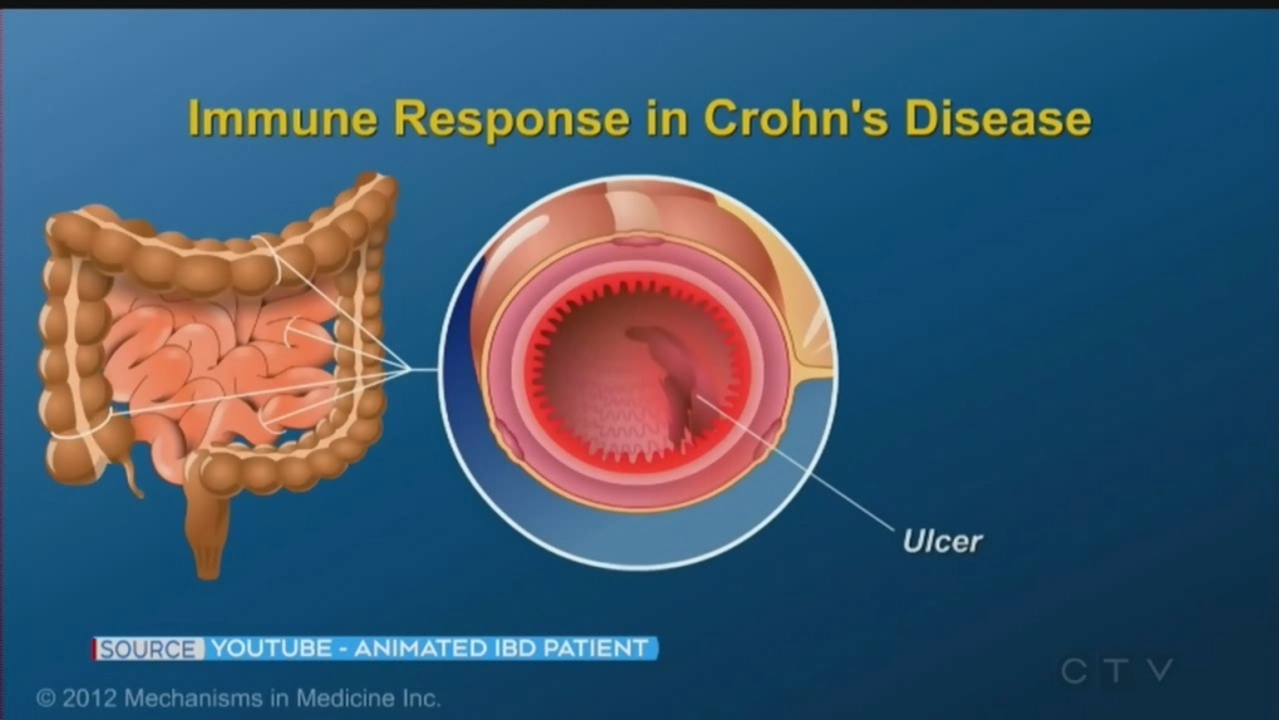
As a blogger, I've recently delved into the connection between chronic diarrhea and Inflammatory Bowel Disease (IBD). I've discovered that chronic diarrhea can be a significant symptom of IBD, as it is caused by inflammation in the digestive tract. This inflammation can lead to various complications, such as pain, malnutrition, and even a higher risk of colon cancer. It's essential for those experiencing persistent diarrhea to consult a medical professional for proper diagnosis and treatment. By managing IBD effectively, patients can relieve their chronic diarrhea and improve overall quality of life.
