Waking up exhausted is something you shouldn't have to live with, yet many people do. You might feel tired all day, even after a full night in bed. This often points to an issue hiding in your sleep, specifically something called Polysomnography, which is technically known as a sleep study. It is a comprehensive diagnostic procedure that records multiple physiological parameters during sleep to identify sleep disorders. When doctors recommend this, they want to see exactly how your body behaves while you try to rest. Understanding the process can take away the anxiety many patients feel before their appointment.
What Is Polysomnography Really?
You might wonder why this test exists when you can just count your sleep hours. The problem is counting time doesn't tell you about quality. Polysomnography captures more than just how long you slept; it monitors your brain waves, heart rhythm, breathing patterns, oxygen levels, and limb movements simultaneously. Think of it as the ultimate health checkup for your sleep system.
The term itself comes from Greek roots: 'poly' meaning many, 'somno' for sleep, and 'graphy' for recording. It reflects the fact that we aren't just looking at one thing. While home tests exist, in-lab sleep studies remain the gold standard because they track every variable at once. Doctors at major institutions rely on this data to spot complex issues that simple breath monitors miss.
The Setup and Sensors Explained
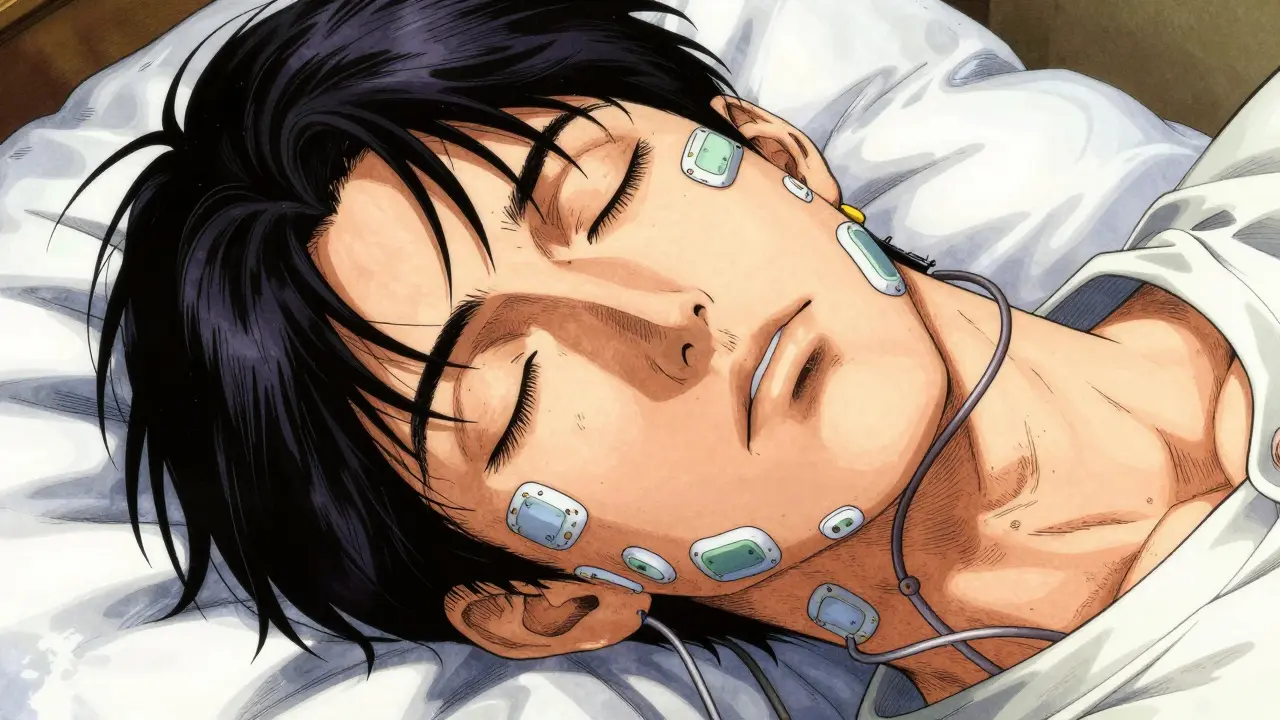
When you arrive at the sleep center, a registered technologist will guide you through the setup. This takes about thirty to forty-five minutes. They attach roughly twenty-two electrodes and sensors to your head, chest, face, and legs. It sounds intimidating, but these wires are soft and flexible.
| Sensor Type | What It Monitors | Placement |
|---|---|---|
| Electroencephalogram (EEG) | Brain wave activity | Scalp |
| Electrooculogram (EOG) | Eye movements | Beneath eyes |
| Electromyogram (EMG) | Muscle tone and leg movements | Chin and calves |
| Pulse Oximeter | Blood oxygen saturation | Finger |
| Airflow Sensor | Breathing interruptions | Nose and mouth |
There is no pain involved. The room looks like a small hotel bedroom, kept cool at around sixty-eight to seventy-two degrees Fahrenheit to help you relax. If you need to use the restroom, you ask the technician, and they unplug you safely. The goal is to get six to eight hours of data, covering both deep non-rapid eye movement sleep and the REM phase where dreaming happens.
Comparing Lab Studies to Home Tests
Many clinics offer home units now, so you might ask if staying overnight is really necessary. Home sleep apnea tests are cheaper and more convenient. However, they typically measure only three or four parameters, mostly focusing on air and oxygen. They cannot diagnose narcolepsy or strange behaviors during sleep. In contrast, sleep study testing in a lab tracks seven to sixteen different signals at once.
In-Lab Polysomnography Pros:
- Records sleep staging (REM vs NREM)
- Detects parasomnias (sleepwalking, seizures)
- Immediate CPAP titration if needed
- Success rate exceeds 90%
Home Sleep Test Pros:
- No overnight facility stay
- Cheaper initial cost
- Comfort of own bed
If you suspect issues beyond simple snoring or heavy daytime fatigue, the laboratory environment provides the depth you need. Experts note that split-night studies allow technicians to treat you immediately if they find severe apnea in the first half of the night.
What Your Results Actually Mean
After the night is over, the hard work begins. A sleep physician spends hours reviewing the recordings. You won't see them all, but you might get the final report days later. The most critical number mentioned is the Apnea-Hypopnea Index, or AHI. This counts how many times your breathing stops per hour of sleep.
An AHI under five means normal breathing. Between five and fifteen indicates mild sleep apnea. Above thirty suggests severe obstruction. But that isn't the only metric. They also look at how much your oxygen dropped during those pauses. If you stop moving or start acting out, that flags conditions like REM behavior disorder. Accurate diagnosis prevents treating the wrong symptom. For instance, central sleep apnea requires different care than the obstructive type where the throat collapses.

Preparing for the Visit
To get the best reading, you should act normal. Don't pull an all-nighter before the test; you actually want to be tired enough to fall asleep quickly. Avoid caffeine after noon on the test day. Wash your hair and don't put any products in it, as oils interfere with the electrode paste. Bring your pajamas and favorite pillow if you think it helps, but remember you'll have wires attached.
The American Academy of Sleep Medicine sets strict standards for these tests to ensure reliability. If you have trouble sleeping in a new place, tell the tech beforehand. Most rooms have soundproof walls to reduce external noise. Sometimes, the unfamiliar setting causes "first night effect," where sleep is lighter than usual, but this rarely ruins the diagnostic ability of the study.
Common Questions About Sleep Studies
Is polysomnography covered by insurance?
Most major insurance plans cover the cost if a doctor prescribes it for diagnosed symptoms. Medicare typically covers eighty percent of the fee when specific clinical criteria are met, such as snoring and daytime sleepiness.
How long does the test take?
The monitoring lasts about six to eight hours overnight. The setup takes another hour before bed, and removal takes about thirty minutes upon waking. Some centers require you to stay until the equipment is removed.
Can I bring family members to the study?
Usually not. Rooms are private and designed for one patient to ensure accurate data without distractions. Partners generally cannot stay in the room during the recording.
What happens if I don't fall asleep?
Technicians monitor you closely. If you wake up frequently, they will try to reattach sensors or calm you down. Even restless sleep provides useful data, though repeating the test might be recommended if less than four hours of sleep was recorded.
Are there risks associated with the sensors?
There are virtually no risks. The electrical signals recorded are passive. Mild skin irritation from adhesive pads is possible but rare. The procedure is non-invasive and safe for children, adults, and seniors alike.


Paul Vanderheiden
March 28, 2026 AT 06:58glad to see people taking sleep seriously it really changes everything when you get that data... i used to think counting hours was enough but waking up tired means something else is going on
hope your test goes smooth because knowing what happens while you drift off makes such a big difference
staying healthy starts right here!
walker texaxsranger
March 29, 2026 AT 06:07polysomnography often misses central apnea nuances unless technician is watching closely... EEG artifacts common with sweat... AHI calculation varies by software version
home units cheaper but lower specificity... insurance codes tricky for reimbursement sometimes
Rohan Kumar
March 31, 2026 AT 00:07wow another day another conspiracy theory about medical tech 🙄😴
honestly just sleep in your own bed its probably fine or whatever they want to sell you... sensors hurt anyway right? lol kidding mostly but why trust the machines more than intuition...
Richard Kubíček
March 31, 2026 AT 04:53Sleep serves as the foundation upon which our daily mental structures are built.
When we ignore the signals sent by our body during the night we risk long term damage.
Medical tools exist not to replace intuition but to clarify hidden biological processes.
The electrodes track brain waves that reveal stages of restoration we cannot feel consciously.
Oxygen saturation levels drop without warning signs visible to the naked eye.
Airflow interruptions happen in cycles that require precise timing to diagnose accurately.
Laboratory settings remove the noise of daily living allowing pure observation.
Home devices cannot catch every variable needed for a complete picture of health.
Understanding REM cycles helps explain why some mornings feel heavier than others.
Muscle tone monitoring detects movements that precede neurological events.
Treating symptoms without finding the root cause wastes time and resources unnecessarily.
Early detection prevents complications associated with untreated respiratory issues.
Cost concerns should not overshadow the value of accurate diagnostic information.
Health investments pay dividends far beyond the immediate financial cost involved.
Peace of mind comes from knowing the exact condition rather than guessing.
We must prioritize internal wellness over external schedules constantly.
True rest requires a clear understanding of how the system functions best.
Rachael Hammond
April 1, 2026 AT 05:45i totally agrue with u abt the part where labs are better cause at home u move around too much...
also my friends said the paste hurts but i think its okay just dont touch ur hair too much before going...
thank u for sharing all this useful info for free!
Debra Brigman
April 1, 2026 AT 19:43The nocturnal tapestry of rest reveals secrets woven deep within the subconscious weave.
Like a silent symphony playing out in the dark corners of the room.
Sensors dance across the skin capturing the rhythm of life itself.
To witness the body at peace is a rare gift indeed.
We become voyagers charting the unknown territory of slumber.
Dreams drift like clouds across the landscape of memory.
Every blink hides a story waiting to be told through data streams.
Awakening is merely the end of the journey not the beginning.
kendra 0712
April 3, 2026 AT 05:00People really need this info out there!!
Sleep quality matters so much for everyone!!! You never realize how vital rest is until it gets tested properly!!!
The tech is amazing and helps so much!!! Stay strong and check your health!!
Tony Yorke
April 4, 2026 AT 22:40the sensor details look accurate